This blog started as a response to a colleague who was calculating using local community vaccination and positive infection rates, using a 90% effectiveness rate for vaccines, and asking about the risks of singing without a mask outside. He calculated the risk of infection to singers as perhaps 0.15% to 0.31%. Is that reasonable?
Risk of what?
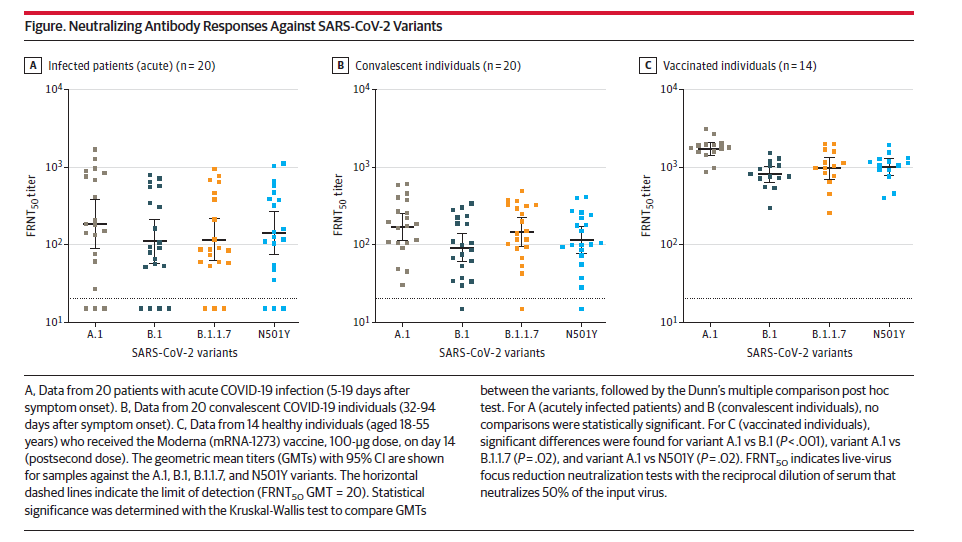
One thing to highlight is that the early effectiveness calculations, and most assertions about the effectiveness of the vaccines being 70-95%, ask whether the vaccines prevented ANY new COVID-19 infections, with or without symptoms, of COVID-19. We now know that if we instead ask whether the vaccines prevent any SERIOUS symptoms (such as a hospitalization or death) of COVID-19 then all three (Pfizer, Moderna, J&J) are well over 99% effective. Here is one link using CDC numbers (red bold text highlights added).
“According to the Centers for Disease Control and Prevention (CDC), 87 million AmericansTrusted Source had received the COVID-19 vaccine as of April 20, 2021. Among vaccinated people, there were 7,157 breakthrough cases, with fewer than 500 hospitalizations and 88 deaths.
Do the math and you can see the cases are about 1/100th of 1 percent of those vaccinated.
“The effectiveness of any vaccine in preventing serious illness is high, and in the case of the COVID-19 vaccines, it’s very high,” Dr. S. Wesley Long, an infectious disease researcher and clinical microbiologist at Houston Methodist in Texas, told Healthline.
“All the data shows that if you’re vaccinated you probably won’t get any symptoms at all, but even if you do, you still probably won’t get full-blown COVID and end up in the hospital,” he said.“
https://www.healthline.com/health-news/covid-19-vaccines-are-more-than-90-effective-what-that-means
So 87,000,000/7157 = 1/12,000 => a 0.008 percent risk of any detected new COVID-19 infection (presumably found through patients seeking care symptoms or anyone receiving testing), and 87,000,000/588=1/147,000 => a 0.0007 percent or death or hospitalization. So that risk is equivalent to less than one person becoming seriously ill in the city of Newton, where I live. These risks are comparable to the extremely low rates of new infections and hospitalizations found in Israel, the first >1 million population country to achieve over 90% (i.e. universal) vaccination for COVID-19.
CDC?
Here is how the CDC website summarizes this research.
“A small percentage of people fully vaccinated against COVID-19 will still develop COVID-19 illness
COVID-19 vaccines are effective. However, a small percentage of people who are fully vaccinated will still get COVID-19 if they are exposed to the virus that causes it. These are called “vaccine breakthrough cases.” This means that while people who have been vaccinated are much less likely to get sick, it may still happen. Experts continue to study how common these cases are.”
https://www.cdc.gov/coronavirus/2019-ncov/vaccines/effectiveness/why-measure-effectiveness/breakthrough-cases.html
I believe the CDC does not want to make a more precise statement such as “less than 0.1 percent risk” instead of “a small percentage” because the CDC wants everyone to get vaccinated. Plus these low rates are in an environment where most people are still wearing masks and social distancing. The rate of breakthrough infections will go up if people stop wearing masks and gather in crowds. Still, the extremely low rates of SERIOUS illness among those who get infected will likely hold, even if by stopping mask-wearing we increase the number of people infected.
So the risk of something serious happening now for a normal healthy vaccinated person is truly minuscule, and when you also note that the prevalence of Influenza this year has been knocked down to close to zero, singing or exercising outside and not wearing a mask inside among vaccinated people seem like acceptable risks for most of us.
Overall risk versus risk from one activity
The above calculations are averages for very large populatinos over the entire period since they were vaccinated, a span of at least a month after full vaccination. We also do not know how much of the reduction is due to having fewer people infectious around you versus lower risk of getting any symptoms when exposed to some virus germs. One assumption is that it is symmetric, in which case the probability of both goes down equally, and the prob of symptoms if vaccinated when exposed to an infectious germ becomes (0.00008)^.5 = .009 and the probabilty of being infectious when vaccinated also become (0.00008)^.5 = .009. Note that .009*.p009=.00008, the overall risk conditional on being vaccinated and when around others who partially vaccinated. I will use this .009 rate below. The fact that this rate is not observed to be getting better suggests that the probability of symptoms when exposed is what is improving the most, but this only strengthens the calculations below.
The probabilities for a given activity, such as singing outdoors or eating inside a restaurant once a week is different since these risks are included in the overall risk calculations. It is hard to attach a probability to any one of these activities. Before precautions, health care workers in China working many hours on patients with covid had very high rates of infection, 70% or more. Similarly spouses of infected people can also have high rates, 70%. And certain wedding, banquet dinner, and Biogen conference attendees also had very high rates of infections 30-50% from single events, conditional on at least one person being highly infectious. So the right calculation is how many people at a given event (e.g., a group of singers singing outdoors) will be highly infectious and how many will they infect, even if we assume exposure would be say 50%. Almost no one who is vaccinated at such an event should be highly infectious. Lets use the conservative assumption that someone in the choir has a breaktrhough infection with certainty, and that they have a 50% chance of infecting a given person. There is still the good news that for a vacinated other singer, the relative risk of a breakaway infection for a healthy person (see above) remains only 0.009. If we again conservatively assume that 100 percent of the risk from exposure is from this one risky activity, then this 0.009 risk can be assigned to this one risky activity. But we still should assume that there is only a 0.5 probability of infection even if the one assumed person is infectious. So my back of the envelope calculation is that a plausible upper bound on the probability of a vacciated person becoming infected from a moderate risk activity when around a known person in the group who is infectious becomes (.009)*(0.5) = .0045. If instead of being around a person with a known infectious rate of 1, we are around a random person, and the average infection rate is 1.5%, then the risk to a fully vaccinated person would be (average infection rate) * (upper bound on risk from one risky activity) = 0.015*0.0045 = 0.00007 => 1/14,000 an upper bound on risk to a vaccinated person of doing a risky activity around random people. Note that this upper bound calculation is assigning 100% of the risk of infection to time spent singing outdoors in a choiror eating indoors at restaurants, which is likely way above (100times?) the true risk. And the risk will be much lower to the extent that the people participating in the activity have more than the average population level of vaccination.
A useful test of these calculations is to look at rates of infection of vaccinated medical staff who are treating COVID-19 patients, or of spouses with an infected partner. For them, the risk using this calculation would be on the order of 0.009, almost one percent, which is high. There will be a literature on these topics. I just have not explored it. Please send me the link if you find them.
Caveats
Unstated in these calculations is that most of the breakthroughs are occurring in people with compromised immune systems. Conditional on getting a detected breakthrough infection, the probability of getting seriously ill is 588/7157=8.2%, and of dying 88/7157=1.1%. These rates are comparable to early rates for random populations before any social distancing or vaccines. This key group remains at high risk even with the COVID-19 vaccine and is worthy of some extra precautions by all of us.
Another important caveat is that these calculations of risk ignore key correlations. The people not getting vaccinated also tend to be people who are reluctant to wear masks, and also more likely to go to bars and large group gatherings where they are at a much higher risk. Predictions using averages will tend to underestimate the true infection rates since these factors compound the risk. And they tell us to avoid these kind of people.
So enjoy Mother’s Day this weekend. If you are fully vaccinated, your risk of infection is very low from normal activities, but your possible exposure to others when not wearing a mask could still endanger them, especially if they are immune compromised. Wear a mask to be sure when around strangers, especially indoors.
Back to research.
Randy